The Use of Mesh in Breast Reconstruction
Mar 21, 2022There are many questions about what mesh is, why it is used, benefits of mesh and what material it is made from. In this article, we will be looking at the use of mesh specifically when used in breast reconstruction. It is also interesting to note what happens to the mesh once it is inside the human body.
Why Is Mesh Used?
On a simplistic front, mesh is used to "bridge a gap" created by the various types of breast reconstructive surgeries.
A "gap" can be created by the insertion of a foreign body, such as an expander or a permanent implant, and the rearranging of internal tissues to accommodate that foreign body. A gap can also be created by removal of tissue, such as during a TRAM flap where portions of the rectus abdominis muscle (your six-pack muscle in your abdomen) has been removed.
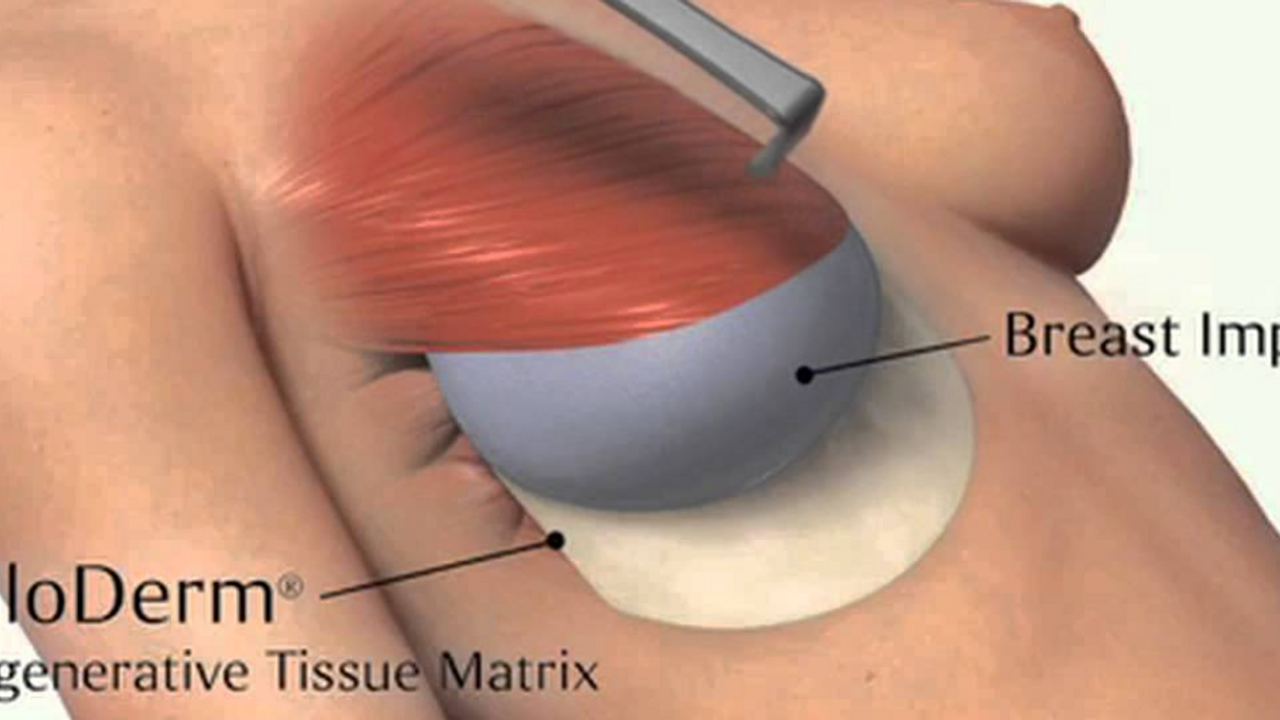
When a "pocket" is created by separating the pectoralis major muscle off the chest wall, to lift it to make a space to insert the prosthesis (whether that be a temporary expander or more permanent implant - permanent meaning it may last more than 10 years) then there gets to be a need for an additional substance to act like a bridge between the inferior and lateral borders of the pec major, since it is sitting in a more elevated position - hence the mesh, which then wraps around the inferior portion of the breast like a demi-bra and holds the prosthesis in place.
Boháč et. al says mesh also helps "control the positioning of the implant in the inframammary fold, and prevents the formation of contractile pseudocapsule around the breast implant" (2018).
Mesh, as a collection of dense fibres, acts as a lattice for the body to revascularize and repopulate with blood supply and immune cells, so in time, it actually becomes an integrated part of the body (Boháč et. al).
Benefits of Mesh:
The same article by Boháč et. al says a mesh reduces the need to elevate the serratus anterior muscle or rectus abdominis fascia for the implant coverage, and can reduce the postoperative pain and local muscular deficits, as well as decrease length of time needed to perform the operation.
An article in the European Journal of Surgical Oncology mentioned the use of mesh allows for a direct-to-implant procedure with greater control over the lower breast pole shape, inframammary fold position, which results in an improved aesthetic outcome post-operatively.
Types of Mesh:
There are two generalized categories of mesh. The first is made of synthetic fibres, and has shown to be more cost effective than mesh harvested from animal or human tissue (Becker).
Synthetic Mesh:
There are several types of synthetic mesh that can be used, and many have a basis of polypropelyne according to an article by Becker, which offers less flexibility and elasticity. According to Creativemechanisms.com, Polypropelyne is a thermoplastic polymer which becomes flexibly at certain temperatures, and stiffens as it cools. Healthline says polypropelyne is derived from petroleum, and is considered by the Environmental Protection Agency (EPA) to be a safer form of plastic. In Becker's article, various combinations of polypropelyne were mentioned, none of which were specifically meant for breast reconstruction.
Towards the end of his article, Becker mentions a product by Durasorb (polydioxanone), which is a "monofilament, long-term absorbable mesh which is fine and flexible and suitable for all aspect of breast surgery" (2020).
Biological Mesh:
Two sources for biological mesh, otherwise known as acellular dermal matrix or ADM for short, are made of porcine (pig) tissue and human tissue. Mesh consists of a swatch of skin with all cells, blood vessels and lymphatic vessels removed, so it is just a clean lattice of collagen fibres.
A study by Chen e. al. said that once the biological tissue had gone through it's preparation process a "histological examinations revealed that the epidermis, dermal fibroblasts, and epidermal appendages were completely removed by these treatments, and the basic dermal architecture of collagen bundles was that of a loose meshwork" (2006).
Boháč stated that ADM was "well-vascularized after several months and become colonized by numerous fibroblasts and myofibroblasts, as well as lymphocytes, macrophages, granulocytes, and mast cells" (2018). In their study, one patient had their expander in for 9 months, and was the only one to show lymph vessels had formed on the side of the ADM that was against the prosthesis, suggesting the lymphaniogenesis is a slower process than aniogenesis.
******
So there you have it, folk. A short overview of mesh, what it is, what it is used for and how it operates once inside the human body.
For more information on mesh and its use in breast surgery, as well has how to treat patients who've had mesh inserted into their body, please look into our Level 1 course for massage therapists "Introduction to Breast Surgery".
References:
Becker, H. Update on the Use of Synthetic Mesh in Reconstructive and Cosmetic Breast Surgery. Aesth Plast Surg 44, 1128–1129 (2020). https://doi.org/10.1007/s00266-020-01767-2
Boháč, M., Danišovič, Ľ., Koller, J., Dragúňová, J., & Varga, I. (2018). What happens to an acellular dermal matrix after implantation in the human body? A histological and electron microscopic study. European journal of histochemistry : EJH, 62(1), 2873. https://doi.org/10.4081/ejh.2018.2873
Creativemechanisms.com - Everything you need to know about polypropelyne (PP) plastic. Retreived March 22/22
Fu, A., Liu, C. Is Pregnancy Following a TRAM or DIEP Flap Safe? A Critical Systematic Review and Meta-analysis. Aesth Plast Surg 45, 2618–2630 (2021). https://doi.org/10.1007/s00266-021-02289-1
Healthline.com - Is Polypropelyne a safe plastic to use in your home? Retrieved March 22/21
Ray-Neng Chen, Hsiu-O Ho, Yu-Ting Tsai, Ming-Thau Sheu,
Process development of an acellular dermal matrix (ADM) for biomedical applications,
Biomaterials, Volume 25, Issue 13, 2004, Pages 2679-2686, ISSN 0142-9612,
https://doi.org/10.1016/j.biomaterials.2003.09.070.
(https://www.sciencedirect.com/science/article/pii/S0142961203007804)
Lisa Whisker, Matthew Barber, Donna Egbeare, Ashu Gandhi, Adam Gilmour, James Harvey, Lee Martin, Rachel Tillett, Shelley Potter . Biological and synthetic mesh assisted breast reconstruction procedures: Joint guidelines from the Association of Breast Surgery and the British Association of Plastic, Reconstructive and Aesthetic Surgeons. VOLUME 47, ISSUE 11, P2807-2813, NOVEMBER 01, 2021. Published:May 25, 2021DOI:https://doi.org/10.1016/j.ejso.2021.05.036




